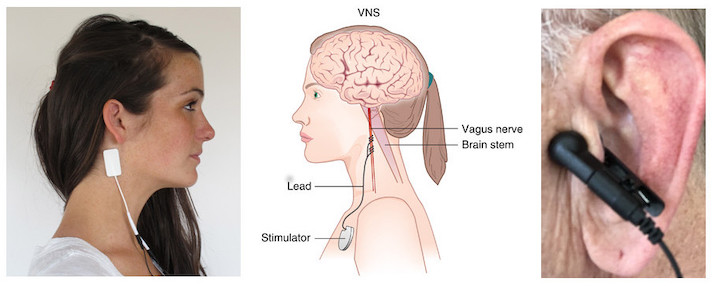
With the increasingly stressful lifestyle there is also rise in other types of disorders such as anxiety and sleep disorders. With the lack of sufficient treatments that address these disorders, cranial electrotherapy stimulation comes as an innovative and required...